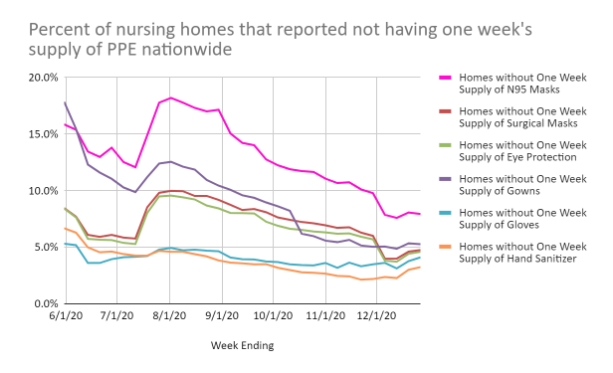
Nursing homes still don’t have enough masks, gowns and other PPE
Shortages improved during the fall but worsened in December

Masks and gloves and hand sanitizer. How difficult can it be?
Here we are, nearly a year government officials after knew COVID-19 was going to be a thing, and nursing homes and others still don’t have enough masks, gloves and other personal protective equipment. There are many complex issues surrounding combatting the coronavirus. Few could have guessed last year that $1 N95 masks and 25-cent gloves would be obstacles.
They were last year, and they still are, according to our latest analysis, which looked at PPE supplies through Dec. 27.
Research last fall by U.S. PIRG Education Fund and Frontier Group found that, in August, 20 percent of nursing homes had dangerously low supplies of one or more types of PPE such as N95 or surgical masks or gowns.
Our new research contains good news and bad news. The good: The shortages of N95 masks, surgical masks, eye protection and gowns were cut in half between late August and late December. Shortages of gloves and hand sanitizer showed smaller improvements.
The bad news: While shortages of surgical masks, eye protection, gowns, gloves and hand sanitizer all declined throughout the fall months, the shortages increased as December went on. Among the six types of PPE nursing homes are supposed to have, only supplies of N95 masks remained stable between November and December. Shortages of hand sanitizer actually increased by 50 percent compared with late November.
The supply issues likely stem in part from the post-Thanksgiving COVID surge and the rollout of vaccinations in mid-December, which require those administering the shots to use PPE.
By late December:
- 8 percent of nursing homes had a critical shortage of N95 masks, which are the best protection against spreading the virus.
- 4 to 6 percent of homes reported shortages in at least one other category: surgical masks, eye protection, gowns or gloves.
- More than 3 percent reported shortages of hand sanitizer, which is much more widely available now in grocery stores and online than it was in the spring and summer.
More COVID relief funding for nursing homes can’t get approved quickly enough. President Biden’s proposed COVID package includes $30 billion for boosting PPE production, and the president promised to invoke the Defense Production Act to help with PPE, which should have been done last spring.
Supplies of PPE are tremendously important for a few reasons:
-
They protect workers in nursing homes, and they protect residents from workers who may have the coronavirus but be asymptomatic.
-
They protect the broader community, where workers may go out to the grocery store, to church, to the pharmacy, etc. and unknowingly spread the virus.
-
They offer workers both protection and peace of mind, which may help keep staff shortages from getting worse. Last month, 23 percent of nursing homes were understaffed in at least one position that takes care of patients.
Shortages of PPE should be at zero. And to get there, nursing home workers shouldn’t have to wear the same masks five days in a row or use garbage bags because they don’t have gowns.

Topics
Authors
Teresa Murray
Consumer Watchdog, PIRG
Teresa directs the Consumer Watchdog office, which looks out for consumers’ health, safety and financial security. Previously, she worked as a journalist covering consumer issues and personal finance for two decades for Ohio’s largest daily newspaper. She received dozens of state and national journalism awards, including Best Columnist in Ohio, a National Headliner Award for coverage of the 2008-09 financial crisis, and a journalism public service award for exposing improper billing practices by Verizon that affected 15 million customers nationwide. Teresa and her husband live in Greater Cleveland and have two sons. She enjoys biking, house projects and music, and serves on her church missions team and stewardship board.
Find Out More
PIRG, health professionals combat COVID-19 misinformation

Massachusetts Vaccine Education: Resource Page
Federal vaccine mandate for nursing homes will save lives