
By The Numbers: Is Maryland on Track to Reopen Safely?
Some people and businesses are feeling intense pressure to resume economic activity, but Maryland’s recent increase in positive COVID-19 cases and limited testing and tracing capacity indicates that we are not ready to begin the process of reopening safely as outlined in Governor Hogan’s Roadmap to Recovery. Here, we’ll look at the numbers that explain why.

As much of the country enters the third month of dealing with the COVID-19 pandemic, communities and states have begun to relax social distancing restrictions and reopen businesses. Some people and businesses are feeling intense pressure to resume economic activity, but Maryland’s recent increase in positive COVID-19 cases and limited testing and tracing capacity indicates that we are not ready to begin the process of reopening safely as outlined in Governor Hogan’s Roadmap to Recovery. Here, we’ll look at the numbers that explain why.
Public health experts and think tanks, including the John Hopkins University Center for Health Security, have drafted various plans for reopening. Most of them agree on a general set of guidelines, though some details differ. Given how much is still unknown about the virus, and because these measures are interactive – for example having a strong contract testing program could lessen the need for testing – there is no one size-fits all “right” game plan for reopening.
The primary tactic for moving forward and safely reopening states falls to a strategy of “Test, trace, and isolate:”
- identify infected individuals through testing;
- identify potential infections by tracing who has come into contact with an infected individual; and,
- isolate infections to stop the spread through the use of quarantines and personal protective equipment.
The minimum criteria identified by the Johns Hopkins public health experts as necessary to effectively implement a test, trace, and isolate strategy while relaxing social distancing guidelines:
- A 14-day decline in new cases;
- Tests for all who need them;
- Health care capacity to safely treat all patients; and
- Public health capacity to conduct contact tracing.
What does “ready to reopen” look like?
When a state has successfully slowed or contained the spread of the novel coronavirus, the trend for new cases and deaths should resemble a “bell” shaped curve. Hawaii is a state that has been very successful in containing the novel coronavirus, due both to the state’s geographic isolation and aggressive measures taken by the state government – such as ordering a 14-day quarantine of all new arrivals to the state. We will use Hawaii as a reference throughout.
So, how is Maryland doing under these standards?
Criterion 1: a 14-day decline in new infections
Maryland: We’re not there yet.
Like many other states, Maryland had begun to flatten the curve. But the rate of new infections has only stabilized, not fallen, meaning that spread has not decreased enough to allow for safe reopening. After some lifted restrictions last week, we had our biggest spike in cases yet, demonstrating the virus is still spreading rapidly.
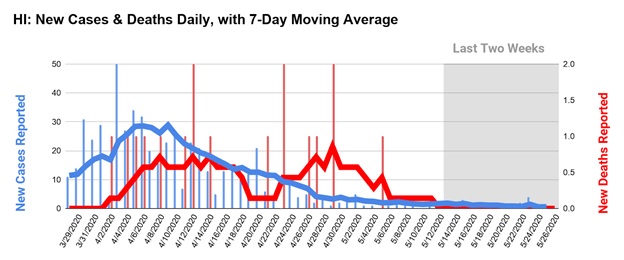
In this graph, the vertical bars represent the daily number of new infections and deaths reported by the state of Hawaii to the Center for Disease Control. The horizontal lines represent the 7-day moving average of each metric. Each point of the moving average is equal to the average number of new cases or deaths that was reported over the preceding seven days, smoothing out variations that may have been caused by testing backlogs and other normal fluctuations in testing numbers.
A state that is ready to reopen should have a graph that looks roughly similar to Hawaii’s: a bell-shaped curve of new infections reported, falling continuously over the last two weeks, with a similar curve of deaths trailing new infections by 1-2 weeks. However, this only works if a state is conducting enough tests to identify most new infections so that close contacts with an infected individual can be notified and quarantined. Ideally, this means that a state should have enough testing capacity to test all essential workers, symptomatic individuals, and possible contacts. Here is that same graph for Maryland. While we saw some decline in the rate of infections prior to lifting some restrictions, it was not consistent over the two weeks defined in the guidelines.
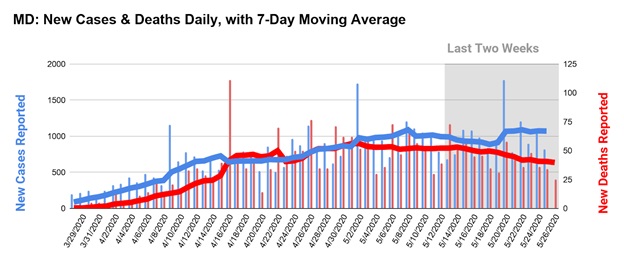
Criterion 2: Tests for everyone who needs them
Maryland: We’re not there yet.
Every state has different circumstances. For example, states with larger populations, larger outbreaks, or higher population density will need a higher volume of testing to accurately identify new outbreaks and contain them. Projections from the Harvard Global Health Institute estimate that Maryland should be conducting almost 28,000 tests per day in order to test all essential workers, symptomatic individuals, and close contacts. At the time the Harvard analysis was published, Maryland was conducting less than 5,000 tests per day. Some days we make it up to 7,000, though testing is being expanded to allow tests for asymptomatic individuals who may have been exposed, which should increase that number. We are not yet testing at the rate we need.
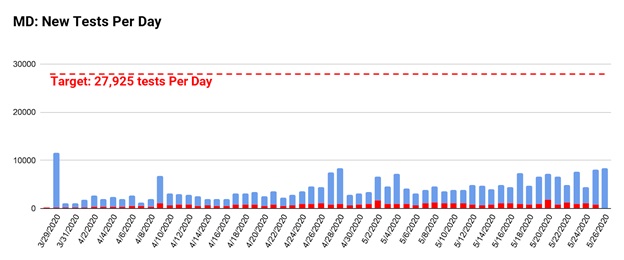
By the same metric, Hawaii, our example state, needs to be able to perform 164 tests per day. The state has far exceeded this goal, with an average of nearly 800 per day.
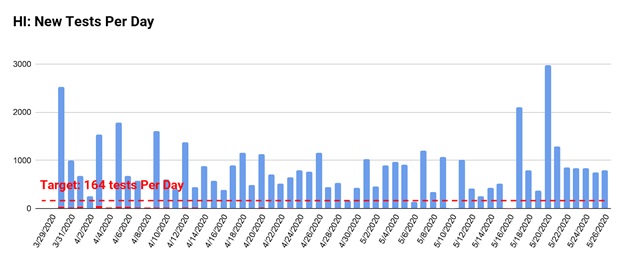
Another metric public health experts use to gauge whether a state is conducting enough testing is the percentage of tests that are returned positive. The World Health Organization puts forth guidance indicating that a state should be able to perform enough tests such that 10% of tests come back positive. A figure less than 10% is considered representative of the larger population, while a figure higher than 10% suggests that many infected individuals are not being tested, making containment –and contact tracing — more difficult.
Hawaii has also been performing well under this benchmark, consistently reporting under 4% positive since April 9th.
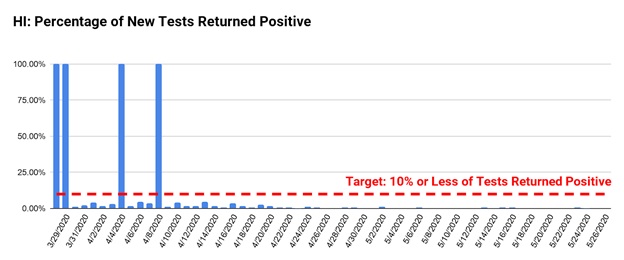
Maryland’s numbers, however, have been fluctuating between 10% and 20% of tests returning positive. The state remains hopeful that that number will decline following the recent expansion of testing.
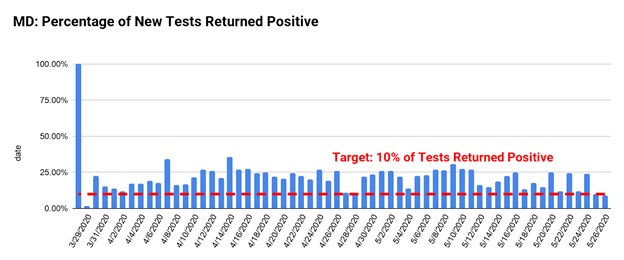
Shortages of testing materials like nasal swabs could also add additional setbacks, and new outbreaks could require a substantial expansion of testing capacity. Maryland PIRG is working with our national partner, USPIRG, to make sure everyone who needs a test, gets a test.
Criterion 3: Sufficient health care capacity
Maryland: We have sufficient capacity, for now
It is important to emphasize that lifting restrictions and reopening businesses will lead to an increase in infections, as we’ve already seen, and until there is a vaccine, this will be the case. Maryland, and other states, should only proceed to reopen if there is enough hospital capacity and personal protective equipment (PPE) available to safely treat COVID-19 patients if there is a surge in new cases. Across the country, there is little consensus on what sufficient surge capacity means precisely — state plans specify the necessary hospital surge capacity anywhere from 20% to 50%.
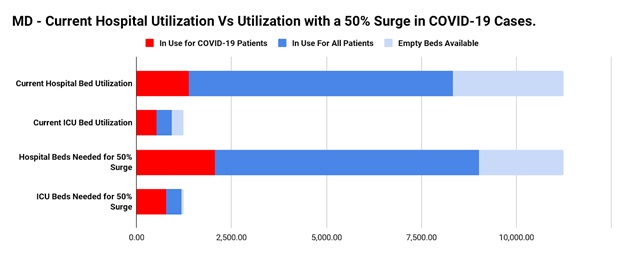
Maryland has a total of just over 11,000 hospital beds. According to the Maryland Department of Health’s latest update on Twitter, almost 1,400 of those are in use for COVID-19 patients, 520 of which are ICU patients. Close to 7,500 more beds are in use for all other patients, leaving around 3,000 available to accommodate a surge. As of now, Maryland meets this requirement, with enough hospital capacity to handle a 50% surge of COVID-19 patients.
In the event of a major outbreak, other issues like new shortages of PPE and ventilators could still occur, and the state should be prepared to reimpose restrictions to preserve health system resources if an outbreak occurs. Maryland PIRG and our national partners have been pushing for greater coordination of medical supplies nationally, and for manufacturers to release technical information on ventilators, so that hospitals can keep equipment operating.
Criterion 4: Public health capacity for contact tracing
Maryland: We’re getting there
States will need to hire hundreds, and in some cases, thousands, of workers to conduct “contact tracing:” identifying the people who have come in contact with a COVID-19-positive individual, and notifying them of their exposure. By first identifying, and then isolating, potentially contagious individuals, an effective contract tracing program can go a long way towards preventing new outbreaks. The National Association of County and City Health Officials estimates that to meet the need for contact tracing during the COVID-19 Pandemic, states will need between 10 and 30 contact tracers per 100,000 population.
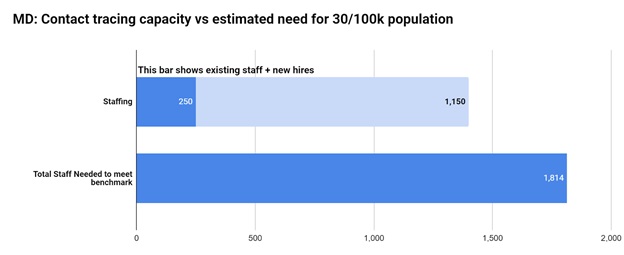
Maryland has a population of just over 6 million people. To meet the benchmark of 30 contact tracers per 100,000 people, the state would need over 1,800 people doing contact tracing work. The State has recently increased its workforce from 250 to over 1,000 to perform COVID-19 contact tracing. The full plan is slated to launch this week, with 1,400 employees able to track 1,000 cases daily — and 10,000 contacts — on a daily basis. Under this plan, Maryland exceeds the baseline benchmark of 10 staff per 100,000 population, but will still fall short of the more thorough 30 per 100,000 benchmark.
Maryland is not ready to reopen
As we only currently meet two of the four public health criteria, Maryland is not ready to begin the reopening process. As we reach some of these benchmarks, however, it may be reasonable to tentatively lift some restrictions to allow some room for increased activity and businesses to get rolling again. As we phase out of restrictions on businesses and activities, some indoor activity and large gatherings (even outdoors) will likely pose too high a risk, but expanding curbside pickup and having limited outdoor social gatherings, could be low risk options.
In Maryland, we have prevented a lot of infections and deaths by staying home and avoided our hospital system being completely overrun. However, we’ve only just gotten our hospital capacity under control and only slowed, not seen a decline in the spread. Maryland’s testing capacity, while growing, lags behind other states. While we are beginning to ramp up a serious contact tracing program, with sufficient staff available to contain new outbreaks, the success of that program is yet to be seen. Until we get testing and our contact tracing capacity up to benchmarks and see a sustained decline in new COVID-like illness, restrictions should remain in place in most of the state.
Topics
Authors
Emily Scarr
State Director, Maryland PIRG; Director, Stop Toxic PFAS Campaign, PIRG
Emily directs strategy, organizational development, research, communications and legislative advocacy for Maryland PIRG. Emily has helped win small donor public financing in Baltimore City, Baltimore County, Howard County, Montgomery County, and Prince George's County. She has played a key role in establishing new state laws to to protect public health by restricting the use of antibiotics on Maryland farms, require testing for lead in school drinking water and restrict the use of toxic flame retardant and PFAS chemicals. Emily also serves on the Executive Committees of the Maryland Fair Elections Coalition and the Maryland Campaign to Keep Antibiotics Working. Emily lives in Baltimore City with her husband, kids, and dog.
Find Out More

With $1,400 payments on the way, here’s what to do, and not do

PFAS Free & I’m Lovin’ It

COVID-19 vaccines, tests and treatments are peddled in new scams
